Prostate Cancer |
||
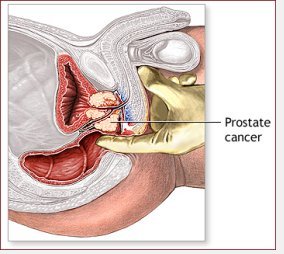
The prostate is a walnut-sized gland below the bladder present in men only. It makes the fluid that carries and nourishes sperm. The prostate sits in front of the rectum ('back passage'), which is why the prostate can be felt by putting a finger into the rectum. Urine flows from the bladder through the prostate to the urethra and then to the outside world. The prostate is like a ring doughnut or polo mint with a hole in the middle.
There are three main problems that affect the prostate: • Prostate enlargement (benign prostatic hyperplasia, BPH), • Prostate cancer • Prostatitis.
If the channel through the prostate gets small as the prostate enlarges, urinary symptoms can develop such as getting up at night, passing urine frequently, or a poor urinary stream. However, the prostate is not the only cause for urinary symptoms. Investigations and treatments for these problems can be found operations for the benign prostate enlargement including laser prostatectomy.
In general, prostate cancer does not cause urinary symptoms unless it is very advanced. Therefore, the majority of men with urinary symptoms do NOT have prostate cancer.
Prostate cancer is a growing problem in this country as men live longer (see graph below). When it starts there are no symptoms, but it is now the second commonest cause of death from cancer in men after lung cancer (see graphs below). Prostate cancer can be detected early using the PSA, PCA3 Score, subsequent prostate biopsies and then deciding what treatment options are best for you including observation. PSA testing is controversial and so it is important to understand the advantages, risks and alternatives to PSA testing. Multiple new treatments have arisen for prostate cancer including HIFU (high intensity focused ultrasound), laparoscopic and robotic prostatectomy.
How do I work out how serious my cancer is?
There are several considerations:
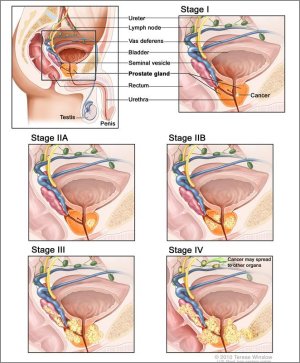
The underlying risk of the cancer is determined principally by: • Gleason Score: this is a measure of how aggressive the cancer is. The two commonest patterns of cancer are each graded from 1 to 5. The two grades are summed and the total is known as the Gleason score. Therefore, this ranges from 2 to 10. Most cancers have a Gleason Score of 6: the most serious is 10 and the best is 6.. • Cancer Stage: This refers to how far the cancer has spread and can be determined partially by prostate examination with a finger, and sometimes with transrectal ultrasound at the time of prostate biopsies, a bone scan or magnetic resonance imaging (MRI) scan. If the cancer is confined to the prostate, the stage is 'T1' or 'T2', if it is outside the prostate it is 'T3' or 'T4'. Bone scans indicate whether there is cancer in the bones. Sometimes, the lymph nodes in the pelvis are sampled laparoscopically to determine if cancer is present there. • PSA: the higher the PSA, the more likely the cancer is outside the prostate; the faster the rate of change, the more likely serious cancer is present • Other bits of information can be used and relate often to the information gained from the prostate biopsies: the proportion of positive biopsies, the length of cancer in the biopsies or the percentage of the core with cancer.
It is important to know how the cancer was detected i.e. by screening with a PSA test or because of symptoms. Most of our knowledge is based on prostate cancer detected in patients with urinary symptoms. If the cancer was detected early because of PSA testing, the time between diagnosis and the development of symptoms from the cancer is likely to be much longer than if the cancer was detected because of urinary symptoms.
What additional tests or scans are necessary now I have prostate cancer?
These tests relate mostly to determining if the cancer is confined to the prostate and what chance there is that treatment will fail after a few years. It is possible to combine the information to calculate whether the cancer has spread outside or the chance that the cancer will return after treatment. The information required is: • PSA • Gleason Score • Clinical stage determined by examination of the prostate by a finger • The proportion of positive biopsies
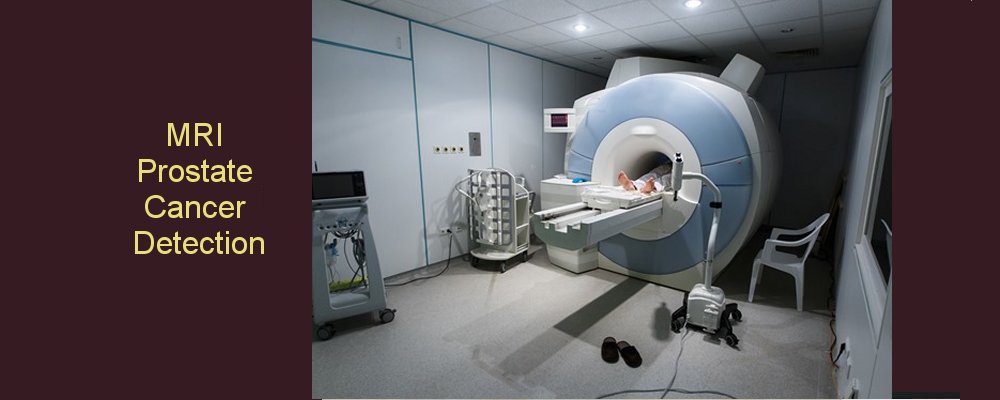
Other investigations, such as magnetic resonance imaging (MRI) can help tell if the cancer is has spread outside the prostate and give information about your anatomy relevant to treatment and side-effects. For this test, you enter a scanning machine, which makes a lot of noise, and produces high quality images of the prostate. It may help determe if the lymph nodes ('lymph glands') contain cancer or not. Sometimes, lymphotropic superparagmagnetic particles are used (this is still under trial). The best way to tell is by laparoscopic lymph node sampling, which is a keyhole procedure for obtaining tissue to examine under the microscope. This is a highly specific test for the identification of cancer in the lymph nodes.
Several websites offer details and on-line help in making decisions including:
Prostate Cancer UK (link) | ||
|
|
Summary |
|