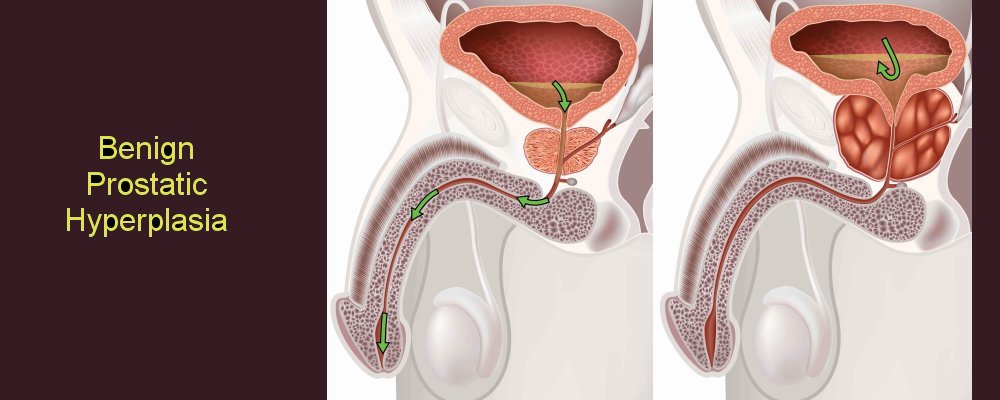
Enlarged ProstateBenign prostatic hyperplasia
|
||
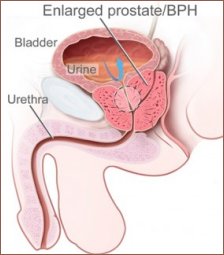
Benign prostatic hypertrophy describes a common condition of the aging male whereby the prostate increases in size and may compress the urethra as it leaves the bladder. This ‘squeezing of the water pipe’ produces numerous urinary symptoms.
Benign prostatic hyperplasia (BPH) with associated lower urinary tract symptoms (LUTS) is a common medical condition in the aging male. The incidence has been estimated to increase from 50% among men between the ages of 50 and 60 years, to 90% for men older than 80 years of age.
In 2016, it is estimated that up to 3 million men in the UK have lower urinary tract symptoms suggestive of BPH. Traditionally the options for treatment begin with making life-style changes for mild symptoms as well as medication.
For operations for benign prostate enlargement see treatments
These include:
Lower Urinary Tract Symptoms (LUTS) This term is used to describe any symptom or set of symptoms arising from the lower urinary tract.
1. STORAGE symptoms
– which are caused by the bladder not acting as an adequate storage organ and include: increased urinary frequency, urgency, nocturia ( getting up at night) and rarely urge incontinence ( or leaking before reaching the toilet),There are three main problems that affect the prostate, prostate enlargement (benign prostatic hyperplasia, BPH), prostate cancer and prostatitis.
2. VOIDING symptoms
– these are caused by a blockage on the way out – slow stream, hesitancy in starting urination, terminal dribble and feeling of incomplete evacuation. The IPSS (International Prostate Symptom Score) is the name for one of these download the questionaire
here The symptoms are graded as: Mild and non bothersome urinary symptoms
If your urinary symptoms are mild (ie IPSS less than or equal to 7 out of 35) and do not cause bother (bother score less than 3 out of 6), then only changes in lifestyle are usually all that is necessary especially if the prostate is small, the PSA is less than 1.5 ng/ml and the bladder empties efficiently. If necessary medication such as an alpha blocker may be given to reduce symptoms. A 5 alpha reductase inhibitor may shrink the prostate over time and reduce the chance of significant problems in the future. Surgery is not usually suggested if the symptoms are mild and respond well to alpha blockers.
If biopsies of the prostate have been taken and inflammation of the prostate was found, there is a greater chance that there may be more problems with either a complete blockage (acute urinary retention) or that surgery may be needed in the future. As such, it is probably sensible to take a 5 alpha reductase inhibitor (e.g. finasteride or dutasteride) as these can reduce the probability of these undesirable outcomes.
Moderate and bothersome urinary symptoms
If the symptoms are more moderate (IPSS between 8 and 19 out of 35) and bothersome (bother score 4 or more out of 6), then treatment by either drugs (alpha blockers), or otherwise surgical options will need to be considered. If alpha blockers have not worked well or the bladder is emptying less well over time, then surgery is recommended. What do I do about having to get up at night?
Getting up at night and passing urine becomes more common as one gets older. Surgery on the prostate may help if the bladder is not emptying completely because of obstruction. However, the prostate is not always the cause of getting up at night. Usually, urine production stops at night, but this may not occur resulting in excess urine production at night. To detect this, keep a record of the total amount of urine passed during the day and night. If the amount of urine made at night is more than 25% of the total daily amount, then the following can help, but discuss with your doctor before adopting the advice below:
Your doctor should advise you further.
Drugs such as alpha blockers (eg tamsulosin or alfuzosin) can also be of benefit. These measures can be combined with a tablet to help encourage more urine production in the afternoon (a diuretic) and something to stop urine production at night (DDAVP).
In some cases, the urgent need to pass urine occurs during the day and night. This problem may be due to overactivity of the bladder muscle and can be helped by avoiding caffeine and taking medicines. These medicines include solifenacin (Vesicare), tolterodine (Detrusitol) and oxybutynin (Lyrinel). When you go to see a specialist ( Urologist), a detailed history will be taken by the doctor including the IPSS score. Examination of the prostate will be carried outy to assess the size and whether it is benign or cancerous.
These tests include the following, but do not necessarily have to be performed always:
|
||
|
|
Summary | |
. |
||
